Foot Ulcer
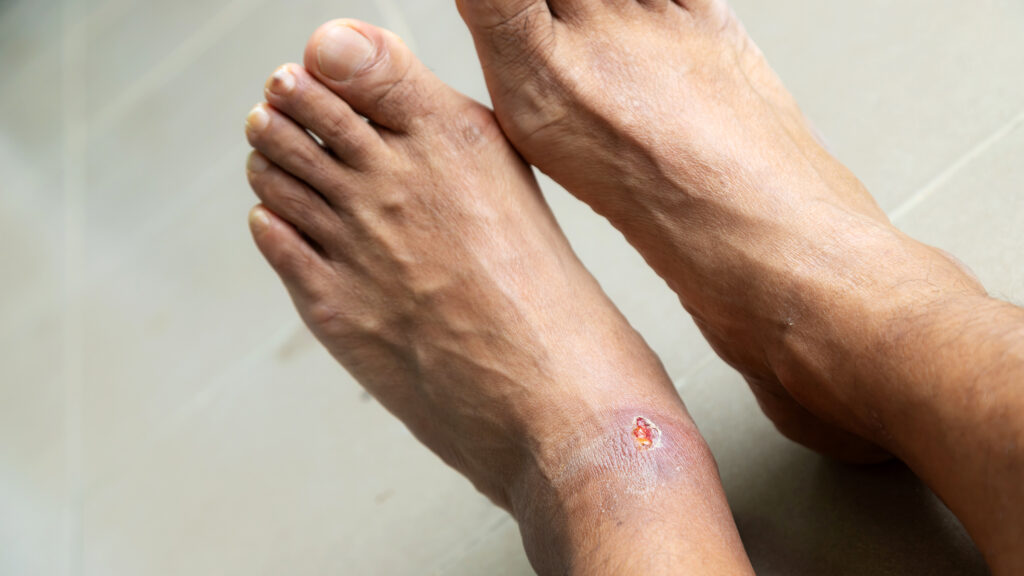
A foot ulcer is an open sore or wound that typically forms on the bottom of the foot, often due to poor circulation, nerve damage, trauma, or infection. It is common in diabetic patients and can become serious if not treated promptly.
Foot ulcers can range from shallow red sores to deep wounds that expose tendons or bone. If untreated, they can lead to serious infections or even amputation.
Symptoms & Treatment
Symptoms of a foot ulcer include redness and swelling around the affected area, discharge or pus, a foul odor, and in severe cases, blackened tissue (necrosis). People with neuropathy might not feel pain even if the ulcer is advanced. You may also notice thickened, callused skin around the wound, or experience tingling, numbness, or temperature changes in the foot.
Foot ulcers are most commonly caused by diabetes, which can lead to both nerve damage (neuropathy) and poor circulation (peripheral artery disease). Other causes and risk factors include smoking, high cholesterol, kidney disease, obesity, poor hygiene, foot deformities, and wearing improper shoes. A small blister or unnoticed injury can escalate into a serious ulcer if not managed quickly, especially in people with poor healing ability.
Diagnosis is typically done through physical examination, but further tests may include wound cultures to detect infection, blood tests, and imaging (like X-ray or MRI) to see if the infection has spread to the bone. If blood flow is suspected to be poor, a Doppler scan or angiography may be recommended.
Treatment involves multiple steps and depends on the ulcer’s severity. First, wound care is essential — this includes cleaning the ulcer regularly, removing dead or infected tissue (called debridement), and applying appropriate dressings. Second, offloading the foot (reducing pressure) is critical. Special footwear, custom orthotics, or even total contact casts may be used. If infection is present, antibiotics will be prescribed — either oral or intravenous depending on how deep the infection has spread.
In severe cases, surgery might be required to remove dead tissue or even infected bone. If circulation is poor, procedures like angioplasty or bypass surgery may be needed to restore blood flow. For diabetic patients, strict blood sugar control is crucial to promote healing and prevent recurrence. A high HbA1c (average blood sugar level) significantly slows down wound healing.
Prevention is always better than cure. People at risk, especially diabetics, should inspect their feet daily, keep them clean and dry, moisturize to avoid cracks, and wear comfortable, well-fitting shoes. Never walk barefoot, even indoors. Nail trimming should be done carefully — preferably by a podiatrist if vision or flexibility is limited. Smoking cessation, healthy diet, regular exercise, and routine foot exams are also highly recommended.
Medical professionals use the Wagner Classification System to grade ulcers from 0 to 5 — from a pre-ulcerous condition (grade 0) to extensive gangrene (grade 5). This grading helps determine the urgency and type of treatment needed.
You should see a doctor immediately if you notice an open wound that doesn’t improve within a week, if there’s redness, swelling, foul odor, or discharge, or if you have a fever alongside foot pain. Timely treatment can prevent complications and preserve your limb and overall health.

Causes and Risk Factors:
High blood sugar levels, nerve damage (neuropathy), and poor circulation associated with diabetes are major contributors to foot ulcers.
Reduced blood flow to the feet can impair healing and increase the risk of ulcer formation.
Neuropathy can cause a loss of sensation in the feet, making it difficult to detect injuries or pressure points that could lead to ulcers.
Conditions like bunions, hammertoe, and high arches can create pressure points that are prone to ulceration.

Dr. Anant Bagul
M.S.Ortho, Specialized Disability Surgeon